There are many skeletal muscle relaxants (SMRs) to choose from when patients need one. We are going to do some comparing and contrasting of these medications, and ultimately, this article will help you identify some of the most important clinical factors to consider when selecting a skeletal muscle relaxant. For your reference, our friends at Pyrls.com have a free comparison chart of 10 SMRs when you sign up for a free account! Below is a sample.
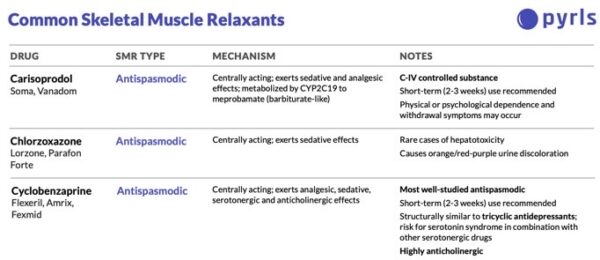
Comparing SMRs – Adverse Effect Profile
One of the most important drug characteristics when comparing skeletal muscle relaxants is anticholinergic activity. Many of the agents in the class carry this risk. This is especially problematic in the geriatric patient population. The most commonly used agents with high anticholinergic activity are cyclobenzaprine and orphenadrine. Generally try to avoid these in patients over the age of 65 or those that may have conditions such as BPH, dementia, or constipation, that may be negatively impacted by anticholinergic medications.
Sedation is another significant adverse effect of these medications. Some skeletal muscle relaxants are worse than others. Metaxalone is the agent that may have a lower risk of sedation than others. I tell you this cautiously because often adverse like this one is dose-dependent.
Another consideration in selection could be blood pressure. If you have a patient who is at high risk of hypotension, staying away from tizanidine would be advisable as it has pharmacologic activity similar to clonidine. I have posted about this in the past demonstrating a classic interaction with ciprofloxacin.
Drug Interactions
When selecting any medication, you have to consider drug interactions. In addition to the adverse effect profile mentioned above, the cumulative anticholinergic burden is an important consideration.
CYP enzymes do not play a huge role in the breakdown of many of these agents, but there are some considerations to assess. If you are ever in doubt, I always recommend running a drug interaction screen. The most significant CYP enzyme to be aware of with tizanidine is CYP1A2. Ciprofloxacin is the most common interaction I have seen in practice when it comes to tizanidine.
Many of these agents also have additive respiratory depression risk with opioids. This is something to educate your patients about as well as try to reduce the opioid burden where possible.
Controlled Substances
Some of the skeletal muscle relaxants are classified as controlled substances. This can certainly sway prescribers in a specific direction. Carisoprodol and diazepam are two of the most commonly used muscle relaxants that are controlled substances.
The risk for withdrawal symptoms exists for many of these agents (controlled or non-controlled). Minimizing the duration of use to a couple of weeks can be really helpful to avoid this risk. If longer-term use has occurred in a patient, it will be important to taper down slowly to have the best potential to wean your patient off of these agents.
Serotonergic Activity of Skeletal Muscle Relaxants
Many patients with corresponding psychiatric issues will also be taking skeletal muscle relaxants for pain management. This leads to a potential issue when using serotonergic drugs like SSRIs, SNRIs, or TCAs. Some SMRs also carry serotonergic activity and can lead to an accumulation of these physiological effects and increase the likelihood of serotonin syndrome. Metaxalone and cyclobenzaprine are the two agents that are most likely to have additive serotonergic activity.
Compelling Indications and Contraindicated Conditions
There are some major disease states to consider when selecting a skeletal muscle relaxant. Seizure risk is the first one I think about. There have been rare associations with seizures in patients taking cyclobenzaprine, so if other options exist in a patient with seizures, it may be best to steer clear of this agent. On the flip side, utilizing a benzodiazepine like diazepam could potentially help reduce the risk of seizure. We do need to be really careful when trying to take a patient off of diazepam who has seizures.
Liver function is another consideration. Many of these agents are recommended to be avoided in patients with liver impairment. In addition, dantrolene (not commonly used) is associated with hepatotoxicity.
There you have it; my major comparisons of some of the most common skeletal muscle relaxants. What else do you consider when recommending or selecting these agents?



0 Comments