A 79 year old female living in a long term care facility was diagnosed with a UTI. Past medical history includes but not limited to urinary incontinence, hypertension, GERD, and osteoarthritis. She has a past history of nitrofurantoin and sulfa allergy.
This patient was initially put on ciprofloxacin to treat the infection. With eventual review of culture and sensitivity reports, it was noted that the bacteria was resistant to ciprofloxacin. The patient was transitioned from the ciprofloxacin to trimethoprim.
Within a day or two of the transition to the new antibiotic (trimethoprim), the patient begins to breakout in a rash affecting a significant portion of her body. Upon investigation of past medical history, the patient had stated that she had taken Bactrim in the past and had a bad rash type reaction. I suspect that this reaction was reported and documented as a sulfa allergy. If you are anything like me, when I see a sulfa allergy, the first thing I think of is Bactrim (which contains sulfamethoxazole). I don’t necessarily think of the trimethoprim component. After this experience, it really emphasized to me the point that if a patient has an allergy to a specific medication, we need to document that. Had the patient had sulfamethoxazole/trimethoprim listed as an allergy (or Bactrim), this would’ve had a better chance of being caught, or at least we’d have the opportunity to more closely monitor.
Looking for more medication mistakes from the frontlines of healthcare? Check out the 30 medication mistakes PDF – it’s free!

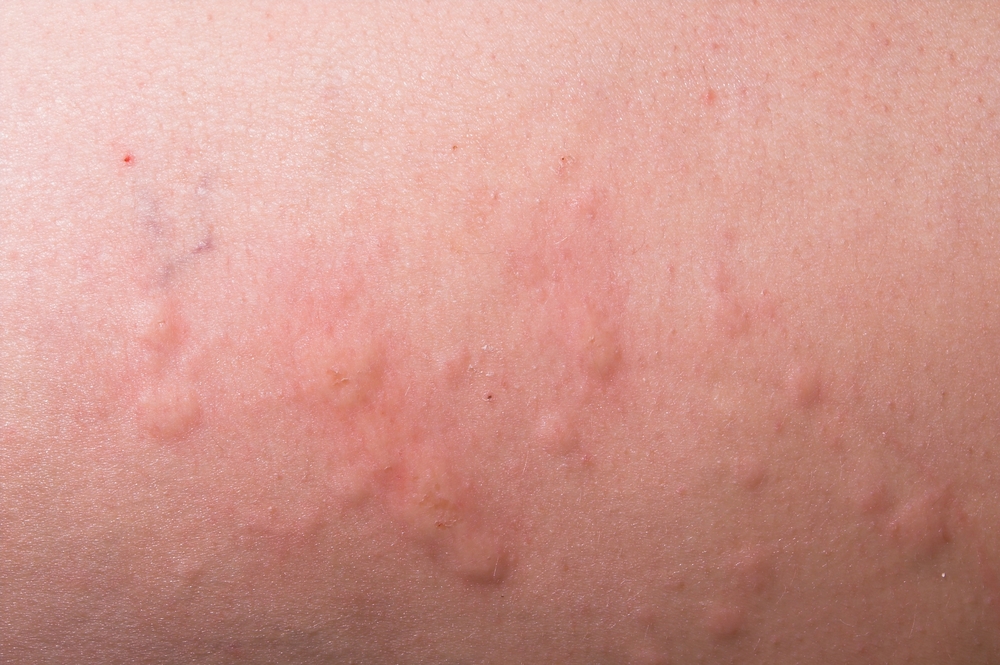

I have seen sulpha allergy.If you saw that reaction you will never think about prescribing Bactrim for a patient
Many software systems don’t offer the ability to screen by drug, they instead screen by generic description of drug class. I have often seen a sulfa allergy marked when it should be an allergy to Bactrim. Occasionally I have seen Bactrim allergy listed in the note field as a clarifier.
The sulphamethoxazole/trimethoprim combination remains a potent and CHEAP antimicrobial agent for respiratory tract and urinogenital infections. The problem is not solved by not prescribing the drug but by taking a proper medication history of the patient. After all this is not the only drug liable to allergic reactions. The experience above underscores the need for pharmacovigilance.
Just make sure the activity director doesn’t have the pt going out for some vit D photo therapy sessions out in the sun!!!