An 87-year-old female is having difficulty with tingling and burning in her feet. She is diagnosed with diabetic neuropathy. Her current medications include:
- Hydrochlorothiazide
- Metformin
- Glipizide
- Tylenol as needed
- Lisinopril
- Aspirin
The primary provider orders gabapentin 300 mg three times daily to help with the new onset neuropathy. The symptoms of neuropathy do begin to resolve, but within a few weeks, the patient is complaining of a new problem.
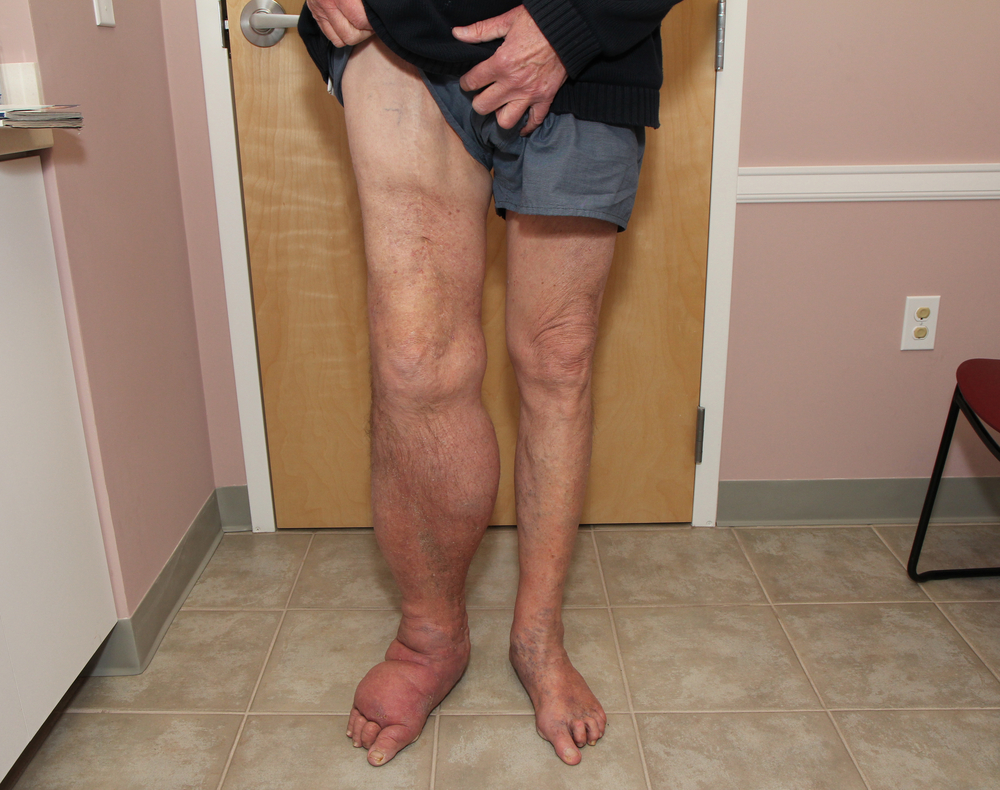
She is noticing a significant amount of swelling in her legs that is greatly frustrating her. She is started on Lasix 20 mg daily to help reduce the swelling. The Lasix (furosemide) does the job of relieving the edema, but now the patient’s new concern is that she is going to the bathroom constantly.
This is the prescribing cascade in action (treating side effects of one medication with another medication). Gabapentin induced the edema causing the addition of more medications. We could certainly go further with this example by adding potassium supplementation and maybe an anticholinergic for urinary frequency from the Lasix etc. In this case, gabapentin was eventually reduced to a lower dose, and this did make the edema less problematic allowing for the discontinuation of the Lasix. I would’ve made the argument that this is a pretty steep dose of gabapentin to begin with in a patient who is 87. Kidney function would be another important parameter to check out in a case like this.
New to the blog? – subscribers get plenty of free education, including 30 medication mistakes I see in my everyday practice as a clinical pharmacist. A simple email address is all that is necessary.


This is a very good example for prescribing errors.I thing this is not doctors inability to know about the side effect of drugs.There are many drugs to start with law dose and gradually increase the dose according to the patient tolerance.Also should check what medication presently they are taking, their conditions of the health etc.etc.Here i will show you a prescription error.The doctor wrote the prescription as follows. Eltroxin .1mg daily.the pharmacist dispensed 10 tablet of 100microgram thyroxine tablets for a single dose.ACTUALLY THIS IS NOT IMAGINATION.If you check this prescription who will be responsible for the mistake.First the pharmacist.The prescriber made the following mistake.He should .He should write Thyroxine 100 micrograms daily in neat and legible letters.Or may be at least he should write Thyroxine o.1mg daily.
Didn’t get u… only mistake of pharmacist…. Pharmacist should there is no single dose of 100 micro of eltroxin 10 tab… he should check with doctor before dispensing
I am a pharmacist too. If the patient had her b12 tested she might have been able to stay off the. Gabapentin in the first place. Metformin induced b12 defieciency could be to blame for the neuropathy also.
On the gabapentin issue. I pt of mine is chronic pain patient, put on gabapentin having sleep walking issues periodically. Was on levaquin last week and they increased. Have you seen this interaction before?
A few years later but I just received this post as my pain mgmt doc put me on gabapentin 2 months ago for nerve pain and damage secondary to a brutal back injury that has required 2 surgeries and we are talking about a 3rd. I am not diabetic and am not overweight. I have had the shakes badly each time he increases the dose. His response is “I’ve never heard of such a thing” but whoop there it is. My 76 year old father with Parkinson’s writes better than I do when this happens. I do take inderal but I’m guessing that not a high enough dose to correct the shaking. So we are back to chasing one med reaction with another. This leg pain is debilitating and so are my tremors; which inderal has taken care of beautifully for 27 years. How can I reach this doctor if he hasn’t even heard of my symptoms?!?!
The shaking is def a side effect of the gabapentin. I was on the highest amount you can take daily for years and had to come off of it because the shaking and tremors got so bad
I am on 3600mg of gabapentin a day i have zero shaking none whatsoever just severe pitted edmea I cannot walk very well even with my walker im only 36 yrs old but I have to be on gabapentin I have severe peripheral neuropathy so I have to be on it nothing else works why dont I get shaking the severe pitted edema in belly lower legs and ankles and feet is all I get and that comes for awhile then goes away its back on fourth im crippled over its awful but still will not stop the gabapentin I need it it a dual thing for me what I need for it works for everything im on it for and nothing else works so I wont stop taking I dont give a sh*t im triple in size because of the severe pitted emdema and the fluid under my feet hurts so bad my skin feels like its going to burst open.
I two get the ahakea randomly .l a. On gavapantin and palexia ,my weight is gaining fast
I am a budding clinical pharmacist from India. I find all information inspiring and educative. Thank you.
thanks, glad it is helpful!
Hello!this also the responsibility of the assigned nurse to check for 7 R’s of medication errors,I know every one is quietly known what they are,so the thing is medication errors are occurring in every where we should counter check the medicine and then go for the pt.Over all our services are zero if we made medication errors , but thanks to you to share your article with us.
There is no mention anywhere in the scenario that there is a nurse administering the meds.
RN, and diabetic for 12 years. I’ll sware by an antidepressant and neurontin – no opioid problem here. Less pain with injections and neuropathy. Never heard of gabapentin induced limb Specific edema. R/O DVT, femoral vain occlusion?? Often seen give in increasing tapered doses 100MG TID in elderly avoids acute sedation. ✌️
I had limb specific edema after starting on gabspentin. Not as bad as the picture, but definitely had it. Stopped gabspentin and it resolved over a couple of weeks. No more swelling. Back on it and thankfully no edema this 2nd tome around.
I have been on gabapentin for years. 800mg, 3 times daily. I’m not having any trouble with Edema or the shakes. This drug is like every drug out there, and effects everyone differently. That’s why there are possible side effects warnings on the informational pamphlet that you get along with your meds at the pharmacist. It’s the patients responsibility to read this information, and decide if the possible side effects are worth the risk. Aspirin is prescribed to millions of people World wide, but just a tiny bit for me can kill me! It sends me into anaphylactic shock. Same with with penicillin, but millions of people use it every day. So you see, everyone’s body chemistry reacts differently. My suggestion, be proactive and read the possible side effects before taking any new medication, and then decide for yourself if the medicine is a right fit for you!
What is the clinical reason for this high dose of gabby?
Lisinopril …not good. Caused sugar to go up.
Glipizide old drug that is not a good drug for diabetes.
Metformin causes neuropathy.. check out vitamin B6 B12 vitamin D and iron levels. These will contribute to neuropathy.
Your meds are making you sick. Those are what I use to take.
So I’ve been on gabapentin about a year now and last month I was diagnosed with cellulitis, at first I thought it was a blood clot. It still burns on occasion but the appearance of it is gone, I was increased slowly and when I got up to 400 mg a day I put on 30 lbs out of nowhere. I’ve also had shingles twice this year and I’m only 41 years old. I am treated for chronic back and neck issues. I want to go off the gabapentin but I’m still dealing with the shingles on my leg and until they are gone I can’t go off gabapentin without extreme pain.
Have you ever looked into Plexus products for the pain..i been on gabepentin for 3yrs. 900mg 3times aday till i started plexus3mo.ago i cut back too twice aday..
Had cancer / major hernia erupted. Gabapentin given but too too much. Could have died. In hospital at the time. Given intravenously. Someone wasn’t watching! Made me really sick with unbelievable headache.
I have been on gabapentin now for well over a year now. At first the doses were low at only 100 mg 3 times a day, then they got increased to 300 mg 3 times a day. I am also on numerous other meds but after the increase I started swelling, mainly on one side which is The side with the neuropathy. My doctor just again increased the dose to 600 mg 3 times a day. Although I can say it has helped with the neuropathy the swelling side effects are not worth taking the increased dose.
I am on Gabapentin but started taking lower doses every 3 month I go down a little..
I can tell when I take it and when i don’t..
It wears off fairly quick and my feet tingle and burn non stop unless I’m moving and I don’t have diabetes.. (tg)
I pray t gis doesn’t happen to me..
I have been on Gabapentin for almost 5 months now and have not had that problem. I take 900 mg 3 times a day. I have gained weight but that has more to due with side effects from my accident, not the medication. I hope everyone’s problems work out!
I have neuropathy from degenerative disk disease at L5-S1, as well as mild herniation at L4-5, which translates into intermittent waxing and waning of severe low back/hip pain which radiates down my anterio-lateral thighs towards my knees. The more I walk of stand, the worse it gets.
I was started on gabapentin and Dr wants me to increase to 900mg TID or 2700mg total daily. I hate taking meds that much, and I’ve have an acute onset of edema and weight gain. I’ve gone from 325# up to 358# and my feet and legs look like water balloons. It MUST be the gabapentin and I can’t tolerate it. I can’t have severe edema and decreased mobility as a side effect of meds that are supposed to help mobility and decrease pain.
Dang, what other options are there?
The issue with Gabapentin although reducing the pain levels if it causes edema therefore more pressure on the nerves which worsens the peripheral neuropathy. It is wise to get B12 B6 levels checked. People can develop B6 toxicity which can worsen peripheral neuropathy. The best way to go is to get with a functional doctor although the downside with that is expenses are out-of-pocket his insurance doesn’t cover medicine that actually works which is ridiculous. A doctor I consulted with was Holly opinionated the less medications the better has all of them or most of them affect the mitochondria and a person needs every cell to be energized to promote healing.
Found all the testimonials here very helpful. The gabapentin I was taking had caused incredible edema in my legs and feet. I am taking 800mg 3x a day = 2400mg. I thought it was odd that my legs were swelling up more than usual. As of tomorrow morning I am weening myself off this garbage while taking lasix to drain the water. I’m getting rid of this edema.
I’ve been on Gabapentin for 12 years for neuropathy in both legs as a result of heavy duty chemo in 2009 at time of breast cancer, mastectomy/reconstruction. 3x a day, 300 mg each. It’s been a life-saver for the pain UNTIL mid-December when swelling began slowly to build in both legs but especially right leg w/ my bum knee scheduled for knee replacement. Within 2 weeks my right leg especially was size of a linebackers w/ incredible searing pain in both, skin tightness, etc,… Lymphedema confirmed. Only now reading these comments concerning Gapapentin did I have any idea that its best explanation of what’s caused it.
Pleeeze…. what are other alternatives to take for neuropathy pain other than Gapapentin?! I’m 3 weeks in receiving therapy from a certified Lymphedema therapist which is helping (ie., being wrapped to move lymph fluids upward out of my legs plus the decompression machine before wrapping) & I’m soon scheduled to be fitted for compression stockings & velcro-wrap “boots” which will replace the therapist’s wrapping. But are there OTHER MEDICATION ALTERNATIVES so I can get completely off the Gabapentin? I greatly appreciate any help you can give!
Hi Susan, past medical history is very important in determining which medication is appropriate for you, and because of that I don’t make specific recommendations to patients in this forum. I would strongly encourage you to go talk to your local pharmacist/physician and discuss options. There are so many great pharmacist professionals out there! Best wishes to you.
My daughter took gabapentin for back issue. After a few days she began to notice painful edema in hands and feet. It has been two months off of it and it has not resolved. Has anyone noticed this?
I am on 1400 mg of gabapentin for restless legs syndrome and it does away with my restless legs plus allows me to sleep at night, otherwise when I sleep on my stomach, which is the only way I can sleep, my thighs hurt and I can’t sleep. I have developed pitting edema in both legs but it is not bad and doesn’t really bother me. Do I really need to come off gabapentin or lower the dose, or can I just live with the edema?
I’ve been on Gabapentin for over a year for chronic back/hip pain that I ironically barely noticed whebn I was working out 15min-3hrs/d bc the muscles in my posterior chain supported a lot of the weight that my bones now carry a much larger portion of, especially towards the tail end of the lockdown. Anyway, after putting on 55lbs do to the sedentary lifestyle and increasing pain, my doctor raised my Gabapentin to 800mg 4times a day up from the previous three times daily, and bam. Within a week a noticed my shoes felt a bit tighter, but honestly, I didn’t think much of it…two weeks ago. Sometime last week I noticed that my ankles, which are normally pretty thin, even after my balloon from 210lbs too 265lbs seemed to be getting a bit wider, with my normally sharp ankle bones seeming to stick out half as much. Yesterday I really took a good look at them, and more importantly, a feel of them, along with my lower leg. Too my surprise, when I straightened out my bare legs the edema was up to just past my knees. A scar from when I fractured my tibia was also VERY visible, whereas a month ago you could barely see it. The skin is so stretched out, I’d guess 1/4″ in that area, that it looks like it did 8 years ago when it was freshly healed.
Needless to say, I stopped taking it last night. My doc is closed, so I figured I could wait a couple more days to call them as I doubt I won’t be in pain I can’t tough out for another 48 hours, and I have plenty of Tylenol, Aspirin and Ibuprofen, heating pads, Icepacks etc etc..Once the swelling subsides I’ll definitely see about going on a different non-narcotic pain medication which should be interesting as my insurance tried to talk me into going to the pain clinic three times already this year even though I’ve haven’t been to the hospital or made any special trips to the doc for pain besides the initial visits over a year ago. I guess it’s just easier to toss someone on some type of Opioid and call it a day.
I’m optimistic that the swelling goes down as quickly as it set in, because even though it doesn’t hurt, it sure looks silly. I am glad I had a pretty good idea what it was, as this was my first search and the first result I clicked on since I wanted to read experiences, not the chemical makeup a white paper for the drug. Again, no real pain in my feet or legs save a little pressure, and as long as I don’t stand or walk for too long my back shouldn’t scream “Stop it dummy!” too often. I also hope there is a solid alternative that works as good as Gabapentin did since it appears I will be working remotely most of the time now and will finally have a chance to get back into the gym on a regular basis, which should help drop some of this extra weight as I build up to tossing around heavy things again. Weird how muscles can actually serve as a pain deterrent in many cases, and I now understand why it can be so difficult for overweight people to get into good shape, which I really didn’t before, so maybe this is a double good thing? I’m a bit more empathetic (not that I was mean, but the “Eat less move more” doesn’t always apply if walking 50 yards has someone stopping to stretch their back for 60-120 seconds, well it’s tough to speed up you metabolism that way!) and I’ll probably be off daily pain medication completely within a ye. And I have these stupid swollen limbs, and a message board to thank for it, though I’m still obviously going to talk to my doctor about it as I don’t want to drop and have a seizure from “Just stopping” because I didn’t get the “Ok” from them first.